COLON CANCERS
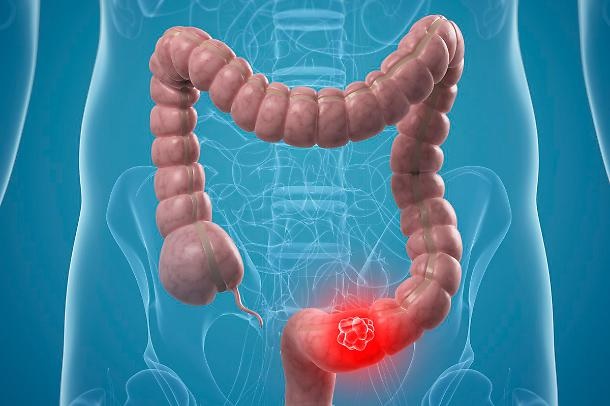
In Europe, colon cancer is the second most frequently diagnosed cancer in both sexes. The most common symptoms range from change in bowel movements (alternating periods of constipation and diarrhea) secondary fatigue to iron-loss anemia and obstructive symptoms in serious cases.
Who is most at risk
- Men and women aged 50 and over (a screening is recommended for the detection of hidden blood in the stool, and a colonoscopy if positive);
- People with family history of colon cancer or colon polyps;
- People with a history of inflammatory bowel disease (e.g. ulcerative colitis and Crohn’s disease);
- Smokers;
- Overweight or obese subjects;
- People who are not physically active;
- People who drink large amounts of alcohol, especially men;
- People who eat a large amount of red meat and especially processed meat (sausages, bacon, hot dogs, salami or other cured meats);
- A healthy lifestyle in accordance with the rules of the World Research Fund can help prevent colon cancer.
How to reduce the risk
A correct primary prevention strategy is necessary. The purpose of primary prevention is to reduce the incidence of cancer by keeping risk factors under control so that the probability of a cancer onset decreases.
Some of the primary prevention strategies can be targeted to the whole population for example proper nutrition or physical activity. Other primary prevention strategies can be aimed at people considered “high risk” for example, people with a high-risk genetic factor or smokers.
Here are some rules for the primary prevention of colon cancer that can be adopted by the whole population:
- Be physically active: exercise for at least 30 minutes a day and for at least 5 days a week;
- Do not drink alcohol;
- Do not smoke;
- Limit the consumption of red meat (beef, pork and mutton). The World Research Fund suggests the consumption of 350-500g of cooked red meat per week;
- Avoid processed meat (sausages, bacon, hot dogs, salami and other cured meats);
- Maintain a healthy weight: avoid becoming overweight or obese;
- Adopt a diet rich in fruit, vegetables, beans and wholegrains;
- Participate in screening programs: periodical fecal occult blood testing.
Medical oncological therapy
Although the occurrence of colon cancer is high, we see a gradual reduction in mortality for both sexes. This is mainly due to the evolution of medical therapy. Chemotherapy is still the best cure that can lengthen the time for a possible recurrence after surgery on the primitive tumor and, in selected cases, lead the patient to recovery.
In recurring and/or inoperable advanced disease, the new molecules such as the anti-EGFR (Epidermal Growth Factor) monoclonal antibodies, the anti-angiogenic drugs belonging to various classes such as the anti-VEGF (anti-Vascular Endothelial Growth Factor antibodies) and small TKI molecules (Tyrosine Kinase Inhibitor), alone or in association with chemotherapy, can turn cancer into a chronic disease.
When the disease is advanced but limited only to the liver, the same drugs are potentially able to make operable what initially was assessed as a non-operable disease and, in selected cases, lead the patient to recovery.
These drugs can cause some side effects which are specific to the drug category for example neurotoxicity, skin toxicity, haematological toxicity, etc. Other side effects are common to all drug categories, for example nausea, diarrhea, constipation. For the latter, there are some recipes on the website to limit their occurrence.
Oncology and Food takes into consideration drugs which have been used in the treatment of pathologies. However, we want to highlight some side effect which are often not taken into consideration by doctors and which can lead to malnutrition in the patient. The symptoms referred to are: dysgeusia (distortion of the sense of taste), iron-deficiency anemia,( fatigue caused by magnesium deficiency and mucositis). These side effects can be alleviated and/or prevented by following easy-to-apply dietary advice found on the website. This advice will complement the drug therapy recommended by your oncologist and will never replace it.